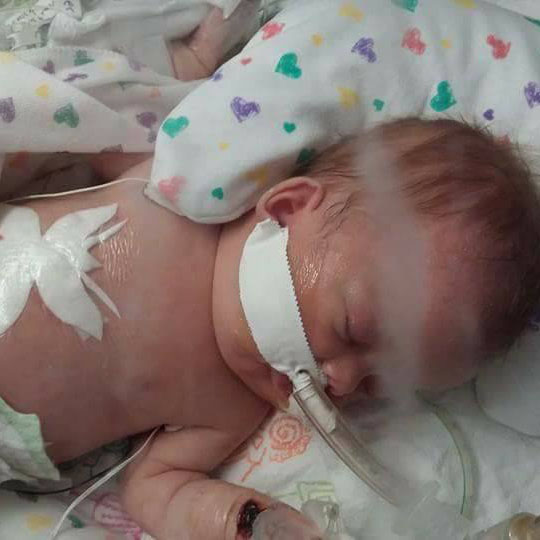
Meet Emily
EMILY'S STORY
Our pregnancy was going swimmingly, we were 27 weeks along with twin girls when a regularly scheduled ultrasound turned everything in our lives upside-down. Like most people, we had never heard of Congenital Diaphragmatic Hernia (CDH), but were quickly sent from our home in Virginia to Children’s Hospital of Philadelphia in order to meet a team of specialists and evaluate our options. We were eventually taken to a small room with a pediatric surgeon, an obstetrician, and a cardiologist who told us that Twin B – “Emily” - had a large right sided diaphragmatic hernia that had allowed her stomach, liver, and intestines to move through her diaphragm into her chest severely restricting her lung growth and heart function. She was given a 3% chance of survival if we could get her to 38 weeks gestation.
If getting to 38 weeks was the plan, reality was much different as I went into preterm labor at 31 weeks in Virginia during a brutal winter storm and transport to Philadelphia was simply not an option. Our local doctor was absolutely amazing but did have to inform us as we prepped for an emergency c-section that Emily would likely not survive the delivery, and even if she did they were unfortunately not equipped to care for a baby with her medical needs at such a small size. Avery was born first and cried as she was rushed to the NICU and Emily followed shortly thereafter. She was born blue, not crying...not breathing. The nurse in the OR placed her ID band on the tray beside me because they do not place bands on stillborn babies. The team worked tirelessly for several hours to stabilize her enough to take her to the NICU where she would stay for the next 17 days until she was stable enough to eventually fly via helicopter to Children's Hospital of Philadelphia. It’s where she would spend the next 100 days of her life.
Emily had her hernia repaired with a Gore-Tex patch at 47 days old, but not before doctors finally allowed me to hold her the very first time the day before her surgery – it was incredibly bittersweet given it was because they simply didn’t know if she would survive the repair. I consider myself lucky though, as my husband wasn’t able to hold her for the first time until two days after her surgery.
Fast forward now five years, Emily just began her third year of Pre-K in preparation for Kindergarten next year, but that doesn't come without risks. She still requires oxygen because her lungs are so small and damaged from trauma associated with her CDH. She’s 100% G-tube fed meaning that all her nutrition goes directly into her stomach, and she does six or more hours of therapy a week to continually assist her development. We continue to travel 3.5 hours from VA to PA to see a team of 14 specialists that give her the best opportunity to thrive and be the best Emily she can be, but this would not be possible without our family, friends, and amazing charities like Fore Hadley!
We were told several times Emily would not survive and that if she did that she would never walk, talk or live life like a normal child – but she is walking, talking proof that deep down in her core she is a fighter and sometimes a 3% chance is all you need!
- As told by Samantha Binns, aka Mom
About the Fore Hadley Angels in the NICU Fund
Support and proceeds for the Fore Hadley Angels in the NICU Fund will go towards assisting current and future families like Alanna’s, by providing financial contributions to assist families with the costs associated with extended, long distance travel and living arrangements. Costs that are often a must to ensure the proper specialty care for CDH babies.